Projects
About the Musculoskeletal Biomechanics Laboratory
Our laboratory investigates the interactions between physical activity and musculoskeletal health. I am particularly interested in how mechanical loads (or lack thereof) can be both beneficial and harmful to bone, and in understanding what conditions influence whether a load helps or hurts a person. I am driven by practical questions: what should I tell my mother or my daughter to do, based on mechanism?
To answer these questions, we apply engineering techniques to translate the basic science work done in small animals to human clinical populations. We work with people on mechanistic clinical trials. Our lab has also developed, refined, and applied techniques to noninvasively measure skeletal structure, loading, and mechanical behavior.
Current Projects
1. Biomechanical and Biological Risk Factors for Metatarsal Bone Stress Injury In Runners
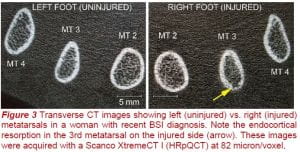
Bone stress injury, commonly called stress fracture, is a common injury in runners. The metatarsals, which are bones in the feet, are a common injury site. Aside from weekly training volume, there are many factors that determine why someone gets injured, such as footwear choice, footstrike biomechanics, and the degree to which a runner may use the muscles in their feet. Our research aims to understand how bones in the feet are loaded during running so that we can improve prevention and treatment for these injuries. This work is in collaboration with Dr. Adam Tenforde at Spaulding Rehabilitation Hospital in Cambridge, and Dr. Irene Davis. You can find more details about the project here.
 We are currently recruiting runners both with and without bone stress injuries in their feet for our research. Are you interested in learning more? Fill out our interest survey here and we’ll contact you.
We are currently recruiting runners both with and without bone stress injuries in their feet for our research. Are you interested in learning more? Fill out our interest survey here and we’ll contact you.
Publications and presentations related to this work:
- Troy KL, Davis IS, Tenforde AS. A Narrative Review of Metatarsal Bone Stress Injury in Athletic Populations: Etiology, Biomechanics, and Management, Physical Medicine and Rehabilitation. Nov;13(11):1281-1290. doi: 10.1002/pmrj.12518.
- Bone architecture and foot muscle strength are not different in healthy male versus female runners. Kyle Murdock, Adam Tenforde, Irene Davis, Karen Troy. (Presented at 2020 ASB meeting) – MTSFX_ASB2020_v3
- Wilzman AR, Tenforde AS, Troy KL, Hunt K, Fogel N, Roche MD, Kraus E, Trikha R, Delp S, Fredericson M. Medical and Biomechanical Risk Factors for Incident Bone Stress Injury in Collegiate Runners: Can Plantar Pressure Predict Injury? Orthop J Sports Med. 2022 Jun 15;10(6):23259671221104793. doi: 10.1177/23259671221104793.
- Hoenig, Tim; Nelson, Evan O; Troy, Karen L; Wolfarth, Bernd; Heiderscheit, Bryan C; Hollander, Karsten; Running-related injury: How long does it take? Feasibility, preliminary evaluation, and German translation of the University of Wisconsin running and recovery index Physical Therapy in Sport 52 204-208; 2021 DOI: 10.1016/j.ptsp.2021.09.007
- AS Tenforde, S DeLuca, AC Wu, KE Ackerman, M Lewis, MJ Rauh, B Heiderscheit, BJ Krabak, E Kraus, W Roberts, KL Troy, MT Barrack. Prevalence and Factors Associated with Bone Stress Injury in Middle School Runners Physical Medicine and Rehabilitation. 12 July 2021 https://doi.org/10.1002/pmrj.12673
2. Bone Health in Individuals with Spinal Cord Injury:
Spinal cord injury (SCI) causes paralysis and as a result, the mechanical stimulation to the skeleton normally provided by muscle activity and weight bearing is severely attenuated. Bone loss is a prominent feature of the immediate post-injury period, however fracture rate does not increase significantly until 5-10 years post-injury. These features make individuals with SCI a model population in which bone adaptive response due to lack of mechanical stimulus may be investigated. Additionally, because the SCI population is at high risk for fractures (similar to that of osteoporotic women), individuals could benefit from interventions that reduce loss of bone mass and strength. Anti-resorptive therapy, a key intervention for osteoporosis, cannot fully ameliorate this problem. Novel therapies and a more complete understanding of the structural changes that occur within the bone of SCI patients would benefit this population.
 Ongoing projects related to bone health in SCI include:
Ongoing projects related to bone health in SCI include:
- Effects of Ekso-Assisted Gait Training on Bone Health and Quality of Life: A Randomized Controlled Trial. This Department of Defense funded clinical trial is a collaborative effort with Leslie Morse, DO, at the University of Minnesota. It is registered at ClinicalTrials.gov NCT02533713.
Publications and presentations related to this work:
- Sex-specific differences in bone mass are maintained following spinal cord injury Courtney M. Mazur, W. Brent Edwards, Ifaz T. Haider, Ying Fang, Leslie R. Morse, Thomas J. Schnitzer, Narina Simonian, Karen L. Troy (2020 ASBMR Annual Meeting) – Mazur_ASBMR_eposter2020_final
- Exoskeleton-Assisted Walking Therapy Increases Muscle Volume in People with Spinal Cord Injury (SCI) Megan P. Pinette1, Nguyen Nguyen2, Ricardo A. Battaglino2, Leslie R. Morse2, Karen L. Troy (2020 ASB Annual Meeting) – Muscle SCI_ASB_poster_v2
3. Designing Exercises to Optimize Bone Health:
We previously found that certain types of strain signals stimulate an osteogenic (bone building) response in adult women. The next question is: how do you design an exercise to build more bone? In this study, we are looking at how changing simple things like jump height, or instructions during exercise, can influence bone strain during the activity.
We are currently recruiting healthy adult volunteers who don’t mind jumping around a bit for us! Are you interested in learning more? Fill out our interest survey here and we’ll contact you!
Publications and presentations related to this work:
- Wilzman AR, Gaudette LW, Troy KL Can unilateral drop landings outperform bilateral in building bone? North American Congress on Biomechanics, August 22-28, 2022, Ottawa, Canada
- Mancuso ME, Wilzman AR, Murdock KE, Troy KL. Effect of external stimuli on human bone: a narrative review. P 2022 Prog. Biomed. Eng. 4 012006 doi: 10.1088/2516-1091/ac41bc
4. Inferring Physical Activity Patterns in Early Humans Based on Bone Morphology
Because bone remodels in response to the specific patterns of strain it experiences, it is likely that endurance running, including differences in footstrike pattern, leaves a reliable signature in human bones, presenting the possibility for inferring locomotive behavior from hominin fossils. This is a collaborative project with Brigitte Holt, PhD, Joseph Hamill, PhD, and graduate student Andrew Best.
Publications related to this work:
- Best A, Holt B, Troy KL, Hamill J. Trabecular bone in the calcaneus of runners. PLoS One, 2017 Dec 27;12(12):e0190553. doi: 10.1371/journal.pone.0190553.
Older/Non-Active Projects
1. Bone Adaptation in Healthy Young Women:
Healthy bone adapts to best resist its habitual mechanical loading environment. When the applied daily mechanical stimulus drops below some minimum threshold, bone loss occurs. Similarly, when the stimulus exceeds some threshold, bone will adapt to become stronger through a combination of increased bone mass and changes to bone geometry that are associated with increased mechanical strength. Our long term goal is to understand how the bone structure and strength in humans are improved in response to physical stimuli. This knowledge is essential for optimizing exercise interventions to prevent fractures by improving bone health. Our research uses experimental data, image analysis, and subject-specific computational models to accurately quantify:
- the mechanical stimulus applied to bone during specific and functional activities
- three-dimensional changes to bone mass, density, and shape that occur over time
- the mechanical consequences of bone adaptation
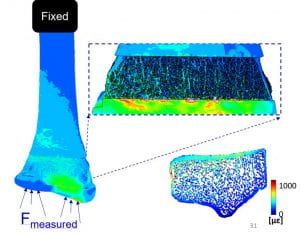 Our NIH-funded investigation (R01 AR063691) focused on:
Our NIH-funded investigation (R01 AR063691) focused on:
- Defining a quantitative input/output relationship between mechanical loading environment and bone adaptation in a healthy skeletal system using a human in vivo distal radius loading model
- Exploring the individual effects of strain magnitude and strain rate on bone adaptation
- Understanding how factors such as physical activity and diet influence bone adaptation
Publications related to this project:
- Troy KL, Mancuso ME, Johnson JE, Butler TA, Ngo BH, Schnitzer TJ (2021). “Dominant and nondominant distal radius microstructure: predictors of asymmetry and effects of a unilateral mechanical loading intervention.” Bone Reports Volume 14, June 2021, 101012
- Mancuso ME, Troy KL. Relating bone strain to local changes in radius microstructure following 12 months of axial forearm loading in women. Journal of Biomechanical Engineering 2020 Aug 26;142(11):111014. doi: 10.1115/1.4048232. PMID: 32844217 PubMed Central PMCID: PMC7580663
- Troy KL, Mancuso ME, Johnson JE, Wu Z, Schnitzer TJ, Butler TA. Bone adaptation in adult women is related to loading dose: a 12-month randomized controlled trial. Journal of Bone and Mineral Research 2020 Jul;35(7):1300-1312 https://doi.org/10.1002/jbmr.3999 PMID: 32154945; PubMed Central PMCID: PMC7363573
- Mancuso ME, Johnson JE, Ahmed SS, Butler TA, Troy KL. Distal radius microstructure and finite element bone strain are related to site-specific mechanical loading and areal bone mineral density in premenopausal women. Bone Rep. 2018 Jun;8:187-194. doi: 10.1016/j.bonr.2018.04.001. PubMed PMID: 29963602; PubMed Central PMCID: PMC6021193.
- Troy KL, Mancuso ME, Butler TA, Johnson JE. Exercise Early and Often: Effects of Physical Activity and Exercise on Women’s Bone Health. Int J Environ Res Public Health. 2018 Apr 28;15(5). doi: 10.3390/ijerph15050878. Review. PubMed PMID: 29710770; PubMed Central PMCID: PMC5981917.
- Johnson JE, Troy KL. Simplified boundary conditions alter cortical-trabecular load sharing at the distal radius; A multiscale finite element analysis. J Biomech. 2018 Jan 3;66:180-185. doi: 10.1016/j.jbiomech.2017.10.036. Epub 2017 Nov 4. PubMed PMID: 29137724; PubMed Central PMCID: PMC5767139.
- Johnson JE, Troy KL. Validation of a new multiscale finite element analysis approach at the distal radius. Med Eng Phys. 2017 Jun;44:16-24. doi: 10.1016/j.medengphy.2017.03.005. Epub 2017 Mar 31. PubMed PMID: 28373011; PubMed Central PMCID: PMC5415424.
- Bhatia VA, Edwards WB, Johnson JE, Troy KL. Short-term bone formation is greatest within high strain regions of the human distal radius: a prospective pilot study. J Biomech Eng. 2015 Jan;137(1). doi: 10.1115/1.4028847. PubMed PMID: 25322335; PubMed Central PMCID: PMC4296241.
- Bhatia VA, Edwards WB, Troy KL. Predicting surface strains at the human distal radius during an in vivo loading task–finite element model validation and application. J Biomech. 2014 Aug 22;47(11):2759-65. doi: 10.1016/j.jbiomech.2014.04.050. Epub 2014 May 9. PubMed PMID: 24882740; PubMed Central PMCID: PMC4248607.
2. Bone Health in Individuals with Spinal Cord Injury:
Spinal cord injury (SCI) causes paralysis and as a result, the mechanical stimulation to the skeleton normally provided by muscle activity and weight bearing is severely attenuated. Bone loss is a prominent feature of the immediate post-injury period, however fracture rate does not increase significantly until 5-10 years post-injury. These features make individuals with SCI a model population in which bone adaptive response due to lack of mechanical stimulus may be investigated. Additionally, because the SCI population is at high risk for fractures (similar to that of osteoporotic women), individuals could benefit from interventions that reduce loss of bone mass and strength. Anti-resorptive therapy, a key intervention for osteoporosis, cannot fully ameliorate this problem. Novel therapies and a more complete understanding of the structural changes that occur within the bone of SCI patients would benefit this population.
Ongoing and recent projects related to bone health in SCI include:
- Skeletal and Clinical Effects of Exoskeleton-Assisted Gait on individuals with chronic spinal cord injury. This Department of Defense funded project is a collaborative effort with Paolo Bonato, PhD, and Leslie Morse, DO, at Spaulding Rehabilitation Hospital in Boston. Doctoral student Ying Fang and research engineer Nate Smith are assisting with this project.
- Clinical trial in collaboration with Thomas J. Schnizter, MD, PhD, at Northwestern University and W. Brent Edwards, PhD at the University of Calgary to test the effect of Teriparatide, vibration, and the combination, on bone mass and bone architecture in chronic spinal cord injury (funded by the Department of Defense).
Publications related to these projects: (see this list)
3. Advanced Imaging to Quantify Joint Deformity in Inflammatory Arthritis
Rheumatoid and Psoriatic Arthritis are two examples of inflammatory arthritis that cause progressive joint degeneration and deformity, especially in the hands and fingers. In this project, we use high resolution CT imaging (HR-pQCT) to develop new methods of quantifying bone erosion and osteophyte formation in these patient populations. The long-term goal is to develop objective and sensitive methods of tracking disease progression, and to provide more sensitive measures to evaluate treatment success. This project wasfunded by a Collaborative Seed Grant between WPI and UMass, and is being completed in collaboration with Ellen Gravallese, MD, and Master’s student Travis Henchie.
Publications related to these projects:
